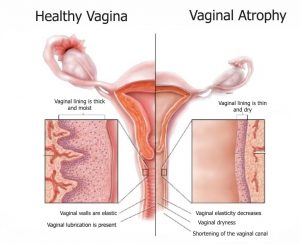
Vaginal Dryness: How Common Is It?
Dryness in the vaginal region can happen to any woman, although, after menopause it becomes more common. A large amount (over half) of post-menopausal women between the ages of 51-60 are affected by vaginal dryness.
We hope that by educating you on vaginal dryness, including its signs, what may be causing it, and the treatments to relieve it, you will feel more comfortable discussing this with your healthcare professional. Knowing that you are not alone in experiencing this frequent problem can inspire you to begin the process of improving your sexual health and life.
Moisture in the Vagina
The natural lubrication of the vagina is produced by the glands at the cervix. The lubricant also helps the vagina stay wet and pliable in addition to keeping it clear of dead cells. Given that it is somewhat acidic and protects against diseases like thrush, vaginal moisture is beneficial for female health. Women frequently have a mild vaginal discharge of white.
When a person is sexually stimulated, two glands called the Bartholin’s glands secrete extra lubrication to help with sexual contact. 16% of women between the ages of 50 and 59 who participated in studies reported experiencing pain or vaginal dryness during sex.
Vaginal Dryness Before Menopause
Even before menopause, 17% of adult women between the ages of 18 and 50 reported experiencing vaginal dryness during sexual engagement. Many women experience this issue because they are not properly aroused during sex, which is often brought on by insufficient foreplay or stress.
Some washing powders, abrasive soaps, feminine sprays, chemicals used in hot tubs and pools, and swimming pools are other causes of vaginal dryness. Vaginal tissues, some antidepressants, allergy medications, cold syrups, and some prescription therapy can also dry out the vagina.
There are several easy methods for lubricating a vagina:
- Simple Lubricants – Just before participating in sexual activity, these lubricants should be administered to the vagina and the area surrounding the vulva.
- Vaginal Moisturizers – These are frequently used a couple of times per week and can last around three days, so they don’t need to be put on right before sexual activity.
For women with low estrogen levels, such as women who have undergone a hysterectomy, breastfeeding mothers, and women who have undergone chemotherapy, vaginal dryness can be a common issue.
Due to a hormonal imbalance, women who are pre-menopausal and have had their ovaries removed after a hysterectomy are more prone to have menopausal symptoms, such as vaginal dryness. Although even women who need a hysterectomy and whose ovaries are still intact will suffer some decline in hormone levels, these differences are more pronounced in women without ovaries since this might make menopause arrive more rapidly.
Chemotherapy-induced hormonal changes in female patients often come on suddenly and dramatically, which makes symptoms worse. Because damaged ovaries can no longer make estrogen as a result of chemotherapy, less vaginal lubrication is created. Additionally, a less elastic and thin vaginal lining results from lower estrogen levels.
After Menopause
Women start to experience physical changes in their bodies after menopause, which normally happens at age 51. The ovaries don’t make the feminine hormone estrogen anymore, and its levels start to decline. An initial sign of decreasing estrogen levels in the vagina is decreased lubrication during sexual activity.
With no synthesis of estrogen, the skin and supporting vulva tissue become thinner and less elastic, with the vagina becoming drier. About 50% of post-menopausal women suffer from dryness of the vagina.
Symptoms
A main symptom is the lack of lubrication and the risk of feeling pain when having sex. After menopause, lubrication issues and uncomfortable sex get worse. Because the vaginal skin is thinner, injury is more likely to occur. This injury can commonly occur during intimacy, especially if the amount of lubrication is insufficient; even a little friction can be uncomfortable and painful. Sexual desire may subsequently decline as a result of painful sexual encounters. Arousal and sexual desire are typically elevated when symptoms are relieved.
Pain at other times: Vaginal dryness can cause discomfort while sitting, standing, exercising, urinating, and even while working. Vaginal dryness can affect daily living for women regardless of whether they engage in sexual activity. This could have a negative impact on people’s quality of life.
A high number of women have also noticed that performing a cervical smear has been more difficult or painful. It is normal for the vulva and vagina to change in appearance; the vagina’s lips will normally be noticeably thinner.
Vaginal discharge changes – a lot of women also mention that their vaginal discharge has changed. It may now be waterier, slightly discolored, and moderately odorous in addition to being irritating and burning. Although these signs may be alarming, they are just a result of hormonal differences and do not indicate a more severe problem.
Women who experience vaginal dryness may experience distress emotionally. It can be hard to accept bodily changes, and the pain and suffering brought on by the illness can make a person lose their sense of self and their sexual confidence.
Given how closely these symptoms match those of thrush or other sexually transmitted infections, many women may find them to be puzzling. Some women buy medication under the incorrect impression that this is a thrush attack, which can worsen the issue.
Given how embarrassing this problem is, many women choose to conceal it, which can seriously erode their relationship, especially if they feel not ready to explain to their partner why they can’t have sex.
Premature Menopause
About 1% of women go through early menopause, which is when menopause begins before the age of 40. It may be a very tough period for a young woman experiencing the significant emotional and physical changes of premature menopause.
Long-term infertility, a condition that is brought on by early menopause, is for many women the most serious aspect of the condition. However, dryness of the vagina can also interfere with a young, energetic woman’s sexual life and relationship with her partner.
A Silent Problem
Even though there are many women who experience vaginal dryness, it is still a taboo topic that people are embarrassed to discuss with partners, friends, or even doctors. Only 25% of female patients with these issues seek therapy.
Because they spend one-third of their lifetime in the post-menopausal stage, women must take care to keep the quality of life they enjoyed before menopause. There are certain things that can be done to stop vaginal dryness from being viewed as a part of aging.
If you suspect that you may have vaginal dryness, be on the lookout for these signs:
- During intercourse, do you notice any irritation, pain, burning, or dryness?
- When having sex or right after, do you ever bleed?
- Has getting your smear gotten more challenging or uncomfortable for you?
- Does the appearance of your vagina look different?
Next Steps
The first step in taking care of yourself is realizing that vaginal dryness is both common and natural. The next step is to speak with a medical professional, who can make a therapy recommendation for you.
- Local estrogen is one option; it comes in waxy pessaries, vaginal rings, gels, creams, or little tablets that are inserted into the vagina. Every three months, the ring should be taken off and replaced. Local estrogen therapy for dryness can aid with pain and discomfort experienced during sex, balance the pH of the vagina, and control germs. Contrary to typical HRT forms, the dangers are small because the effects are local.
- Dehydroepiandrosterone (DHEA) is a once-daily oral spray.
- Ospemifene is a tablet medication that, when taken orally, has an effect similar to that of estrogen within the vagina.
- Women that are not eligible for vaginal estrogen should avoid fragrant soaps and address skin irritation with creams. Particularly for females that are not candidates for estrogen replacement, lubricants and moisturizers can be helpful.
- Slow down the process during sexual contact to give the Bartholin’s gland more chance to make the most lubricant possible.
How to Talk to Your Doctor About Dryness of the Vagina
It can be intimidating to bring up this topic with a healthcare provider (HCP), but it is frequently worthwhile because they can often assist. Here are some suggestions to keep the conversation as simple as possible:
- List the topics you would like to talk about.
- Start by talking about the most significant or challenging issues.
- Record the advice your physician gives you.
- Request clarification if anything doesn’t make sense.
- If you’re feeling self-conscious, do research and bring this along. It can be awkward to bring up unpleasant issues in person, but if you research your symptoms online, you can bring up that information to explain and even avoid making eye contact.
- If you’re still hesitant to bring up the matter, write everything down and give it to the professional.
- Provide the HCP with any information you deem pertinent before waiting to be prompted, such as the background of the ailment, any symptoms you are experiencing, how they are affecting you, any variables related to your lifestyle that may have caused it, and any medications you are now taking.
- If you have any of the symptoms listed above, talk with a nurse about them and request for further details and advice about your condition. Many women notice that getting their smears done becomes more challenging.
In Summary
- Dryness of the vagina is a highly frequent issue that affects over half of women after menopause, however, there are women who may have vaginal dryness issues before menopause.
- Dryness of the vagina is a painful ailment that may affect one’s relationships and life quality.
- There are some simple and efficient therapies for treating vaginal dryness.
- Although vaginal dryness might be an embarrassment, it must be treated, so it is important to discuss your symptoms and causes with your doctor and your spouse.